A National Center for Health Statistics (NCHS) report from 2019 shows 58.9% of Americans over 18 have experienced pain in the last three months [1].
Pain thwarts our work productivity and impairs our quality of life. It affects some groups more frequently than others — women and older adults report the highest pain occurrences.
Below, we’ll discuss chronic pain and who’s most susceptible to having it. We’ll also go through some potential causes and provide data on the prevalence of pain in the US.
What is Chronic Pain?
When pain persists, it can be highly debilitating. John Hopkins Medicine defines chronic pain as “long-standing pain that persists beyond the usual recovery period or occurs along with a chronic health condition.”
Chronic pain can persist anywhere on the body, often due to an injury or illness. However, some people experience chronic pain without any apparent cause.
Related: 10 Types of Pain & How They Differ
Common Kinds of Chronic Pain
Here are the most common locations for chronic pain:
- Back (39.0%)
- Lower limb (36.5%)
- Upper limb (30.7%)
- Headache or migraine (22.4%)
- Abdominal, pelvic, or genital (9.8%)
- Tooth or jaw (9.2%) [1]
Back pain is the most common form of chronic pain. The curvature of the spine — especially in the lower back or lumbar spine — makes the back particularly prone to discomfort.
Our spines are composed of vertebral bones stacked on top of one another with discs resembling cartilage. Below this is our lumbar spine, which experiences the most pressure and strain, as it supports the majority of the weight of our upper body. This is a key reason why posture is important.
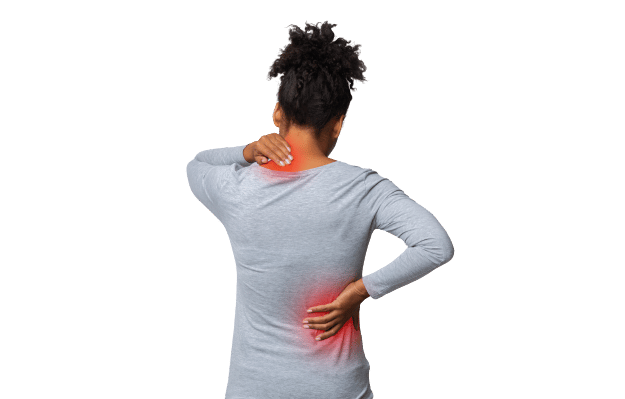
Over time, strain and wear accumulating on this area become ongoing — occasionally chronic — pain.
Additional causes of persistent back pain include:
- Bulging or slipped discs — Often from straining the back through weightlifting
- Spinal stenosis — When the spaces in the spine compress the nerves and vertebrae
- Osteoporosis — Degradation of the density and integrity of bone tissue
- Soft-tissue injury — Often from stress to back muscles, ligaments, or tendons
- Spinal fractures
- Scoliosis
- Lordosis
Any body part can experience chronic pain, but it tends to occur in specific areas.
Below are the most common types of chronic pain among adults:
- Arthritis (joint pain)
- Low back pain
- Headaches or migraines
- Neck pain
- Fibromyalgia (muscle pain throughout the body)
- Pain resulting from nerve damage
- Pain due to cancer
- Carpal tunnel
- Psychosomatic pain (pain caused by a mental factor)
Who Experiences the Most Pain?
Even though chronic pain can affect anybody, research shows the following specific subgroups are more likely to suffer:
Aging Adults
Chronic pain is especially prevalent among people 65 and older. The most common form is knee, hip, and lower back pain due to osteoarthritis or osteoporosis.
Chronic back pain in this age bracket relates to the natural deterioration of intervertebral discs associated with advancing years [2]. According to the NCHS, the prevalence of adult back pain rose with age, from 28.4% for 18-29 year-olds to 35.2% among 30-44, 44.3% among persons 45-64, and 45.6% among 65 and above [1].
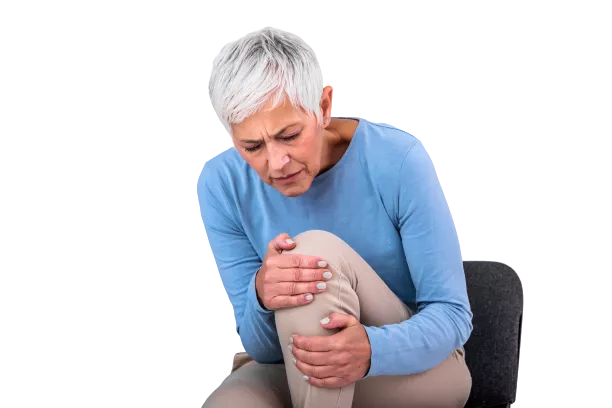
Upper limb pain, lower limb pain, persistent migraines, and other forms of chronic pain are also more common in older people.
Osteoarthritis is one of the most common causes of long-term pain and disability in older populations [3], likely due to accumulated extra fat over time and the natural deterioration of connective tissues.
Persons Living Below the Poverty Line
People living in poverty are more likely to have chronic pain as they are more exposed to environmental dangers, have less access to nutritious food and safe locations to exercise, and have fewer resources for stress management.
Poverty is a stressful situation. It can take a toll on your physical and emotional well-being. A Brookings University study found those in poverty are twice as likely to report chronic pain than those with annual earnings above $75,000 [4].
Living below the federal poverty line increases stress due to worrying about basic needs. Problems associated with poor neighborhoods, debt, limited social opportunities, and a lack of access to medical treatment also exacerbate the concern.

Chronic pain can also be psychosomatic — physical manifestations of emotional distress. By having more problems, people living in poverty are more likely to experience this effect or have it worsen other pain.
Those who endure chronic pain are also more likely to have lower annual earnings. As a result, this cycle perpetuates both poverty and suffering, continually bolstering each other.
Inactive People
Inactivity can lead to muscular atrophy and weakness. Deconditioning and loss of muscle mass increase the risk of developing chronic pain after resuming activity.
Weight gain — a byproduct of inactivity — can also worsen the problem. Fat imposes additional stress on our muscles, joints, tendons, and ligaments and contributes to chronic pain symptoms.
An active lifestyle is one of the best preventative measures for living with chronic pain.
Women
Research shows more women suffer from acute, persistent, and frequent pain than men. Many pain conditions are more prevalent among women than men.
For instance, most people diagnosed with fibromyalgia — a condition resulting in widespread pain in the body — are women. Women also have a higher prevalence of pain-related illnesses like:
- Migraine headaches
- Irritable bowel syndrome (IBS)
- Rheumatoid arthritis
- Osteoarthritis
- Chronic pelvic pain

Although women report higher pain levels than men, they are less likely to seek treatment for their discomfort [5]. Women also wait longer in emergency rooms before receiving treatment [6] and are less likely to get adequate pain medications than men [7].
Common Treatments For Chronic Pain
There are several treatments for chronic pain, ranging from non-steroidal anti-inflammatory drugs (NSAIDs) to prescription painkillers and physical therapy. A doctor will best determine the correct treatments for each condition.
Over-the-Counter (OTC) Medicine
Most people first turn to OTC medications for chronic pain since it often begins as acute pain — the main distinction being that the latter lasts less than four weeks. OTC medicines are more accessible and often less risky than other treatments.
The following is a list of some of the most common OTC drugs for both acute and chronic pain:
- Acetaminophen (Tylenol)
- Aspirin
- Ibuprofen (Advil, Motrin)
- Naproxen (Aleve)

OTC pain relievers only provide temporary relief and are not a permanent fix to an ongoing situation. People with chronic pain should see a physician for the most effective course of therapy whenever feasible.
Prescription Medicine
Prescription pain medication offers more effective relief than OTC medications but with increased side effects and the risk of dependency. The most common prescription drugs used to treat chronic pain are opioids and antidepressants.
Opioids are pain-relieving drugs that can relieve persistent and severe pain conditions like uncontrolled arthritis or cancer. It includes medications such as morphine, codeine, oxycodone, and fentanyl.
Opioids work by stimulating the release of endorphins — hormones that improve our mood — and block our perception of pain. Taking more can increase tolerance, resulting in higher doses and potential abuse.
Physical Therapy & Chiropractic Medicine
Physical therapy and chiropractic medicine might help manage pain in specific areas. These treatments utilize OTC or prescription medications for greater efficacy.
Physical therapy often involves exercise programs like stretching and modalities like ultrasound, massage therapy, and heat therapy. These help decrease inflammation, increase circulation, and relieve muscular tension.

People with musculoskeletal injuries or illnesses — including back pain, neck discomfort, joint pain, and muscular pain — are most likely to benefit.
Chiropractic treatment is a non-surgical form of pain management that involves manipulating joints and the spine to reduce inflammation and muscle tension. Those suffering from spine conditions like sciatica, whiplash, degenerative disc disease, kyphosis, and spondylosis are most likely to benefit from chiropractic treatments.
Alternative Medicine
Some patients are turning to alternative medicine after being dissatisfied with traditional treatment. Some prefer it, considering it is more natural, non-toxic, and has fewer side effects.
Many forms of alternative medicine have been around for centuries. Numerous studies show complementary therapies like acupuncture, yoga, hypnosis, or using substances like cannabis or frankincense can help treat chronic pain.
It may also help avoid the side effects associated with opioid therapy.
Even if detractors claim any relief from alternative medicine is psychological, anything that helps chronic pain go away is an effective solution.
Kratom for Chronic Pain
Over the last few years, another substance has garnered attention for its purported effects on pain. Kratom, or Mitragyna speciosa, is a tree that flourishes in Southeast Asia. Historically, cultures used kratom to ease pain by drying, crushing, and consuming it as a powder or mixing it into a drink [8].
It contains the alkaloids mitragynine and 7-hydroxymitragynine, which interact with opioid receptors, blocking signals in the central nervous system (CNS) [9]. Kratom also provides euphoria, lessening mental distress, including the anxiety and depression from chronic pain.

Kratom interacts with the body similarly to opioids but in very different ways. While it may not be as effective as a medical solution, many consider it a safer option because of its lower potential for addiction and overdose.
Kratom dependence is still possible but is less severe than the dependence brought on by prolonged use of opioids.
For more information on using kratom for pain, read our aptly-named guide, “Best Kratom for Pain Relief.”
Wrapping Up
Chronic pain is a daily part of life for many of the population and is more widespread than many realize. Back pain continues to be the most prevalent cause, followed by pain in the limbs, head and neck, abdomen, genitals, teeth, and jaw.
Chronic pain may be more apparent if you have suffered traumatic injuries, muscular strain, or psychosomatic disorders. The elderly, women, and those living below the federal poverty line are all more likely to experience and suffer from chronic pain.
Many solutions and treatments exist for chronic pain to help alleviate symptoms. OTC medications are available, as are more potent opioids that a doctor prescribes. Physical therapy, chiropractic care, complementary therapies, and all-natural treatments like kratom may also help.
Please consult your doctor if you are experiencing pain for over three months.
- Lucas, J. W., Connor, E. M., & Bose, J. (2021). Back, lower limb, and upper limb pain among US adults, 2019.
- Lan, T., Shen, Z., Yan, B., & Chen, J. (2021). New insights into the interplay between miRNAs and autophagy in the aging of intervertebral discs. Aging research reviews, 65, 101227.
- Dagnino, A., & Campos, M. M. (2022). Chronic pain in the elderly: mechanisms and perspectives. Frontiers in Human Neuroscience, 16, 68.
- Graham, C. (2015). The high costs of being poor in America: Stress, pain, and worry. Brookings.
- Cameron, K. A., Song, J., Manheim, L. M., & Dunlop, D. D. (2010). Gender disparities in health and healthcare use among older adults. Journal of women’s health, 19(9), 1643-1650.
- Hoffmann, D. E., & Tarzian, A. J. (2001). The girl who cried pain: a bias against women in the treatment of pain. The Journal of Law, Medicine & Ethics, 28(4_suppl), 13-27.
- Calderone, K. L. (1990). The influence of gender on the frequency of pain and sedative medication administered to postoperative patients. Sex Roles, 23.
- Cinosi, E., Martinotti, G., Simonato, P., Singh, D., Demetrovics, Z., Roman-Urrestarazu, A., … & Corazza, O. (2015). Following “the roots” of Kratom (Mitragyna speciosa): the evolution of an enhancer from a traditional use to increase work and productivity in Southeast Asia to a recreational psychoactive drug in western countries. BioMed research international, 2015.
- Suhaimi, F. W., Yusoff, N. H., Hassan, R., Mansor, S. M., Navaratnam, V., Müller, C. P., & Hassan, Z. (2016). Neurobiology of Kratom and its main alkaloid mitragynine. Brain research bulletin, 126, 29-40.









