What Is Considered Chronic Pain?
First, you may be wondering how ordinary experiences with pain differ from chronic pain. Medically speaking, pain is chronic when it lasts for longer than three months. Chronic pain can occur anywhere in the body, and while it often gets triggered by a traumatic event — like a car accident or a slip-and-fall — it can also crop up without an obvious stimulus.
Chronic pain is a serious issue, not only because it means living with constant pain but also because it can interfere with normal daily activities. Depending on where the pain is in your body, it could prevent you from walking comfortably, sitting for long periods to work, or even sleeping.
Common Types of Chronic Pain
While chronic pain can occur anywhere in the body for many reasons, some instances are more common than others, and some ailments are more likely to cause it.
Below is a brief list of the most common impetuses related to chronic pain.
- Arthritis (joint pain)
- Low back pain
- Long-lasting headaches or migraines
- Neck pain
- Fibromyalgia (muscle pain throughout the body)
- Pain resulting from nerve damage
- Pain due to cancer
- Carpal tunnel
- Psychosomatic pain (triggered by anxiety or stress rather than a physical issue)
The Biggest Factor In Chronic Pain: Age
Unfortunately, chronic pain is most commonly experienced by older individuals, specifically those over 65. The occurrence of chronic back pain is much higher in this age group, in particular. A collection of studies show 75% of all individuals over 65 deal with chronic back pain [1]. The figures were significantly lower for all other age groups.
Other types of chronic pain — upper limb pain, lower limb pain, chronic migraines, etc. — are also higher in this age group. However, the disparity is lower in most of these categories than in reports of chronic back pain, specifically.
Arthritis is one of the leading causes of chronic pain. Unsurprisingly, osteoarthritis is far more common in elderly populations than in any other age group [2]. Therefore, arthritis could be a leading cause of chronic pain in older individuals.

Other Factors That Affect the Likelihood of Chronic Pain
Chronic pain is, surprisingly, somewhat discerning in who it affects. While any individual of any age group, nationality, and income level can experience chronic pain, several sub-groups of people are more likely to experience it. We’ll discuss these below.
Physical Activity
Individuals who are more physically active are less likely to experience chronic pain overall [3]. Researchers believe this could be because the central nervous system gets accustomed to “comfort” and then overreacts to any kind of unusual stimulus.
Others believe that physical activity tends to reduce the risk of chronic pain because it increases blood flow to joints and muscles, which naturally keeps them healthy.
Whatever the reason, individuals who remain active — even in the face of certain types of pain that don’t indicate damage to the body — are less likely to experience chronic pain throughout their lives.
Of course, intense physical activity can lead to injury that causes acute pain that persists and becomes classified as chronic pain. Still, the risk of chronic pain is lower for active individuals.
Poverty
Somewhat unexpectedly, chronic pain is reported more often by individuals living under the federal poverty line than those living above it. According to a study by Brookings University, chronic pain is twice as likely to be reported by individuals living in poverty than those with incomes topping $75,000 per year.
The stress and anxiety associated with living below the federal poverty line may be the impetus for the high levels of chronic pain within the socioeconomic group. As mentioned above, psychosomatic pain is caused by psychological distress rather than a distinct physical injury or traumatic event.
Unfortunately, those who live below the poverty line are more likely to experience chronic pain, and those who live with chronic pain are more likely to earn less money per year. This creates a positive feedback loop that perpetuates both poverty and chronic pain in many individuals.
Career
Finally, the careers held by individuals can also affect the risk of chronic pain in several ways. This is somewhat unsurprising, especially given the above two triggers for chronic pain.
Individuals who lead sedentary lives and work desk jobs are more likely to experience chronic pain. Similarly, careers that provide an income below the federal poverty line are more likely to trigger chronic pain in individuals. Careers with a high degree of stress can also lead to a higher risk of developing chronic pain.
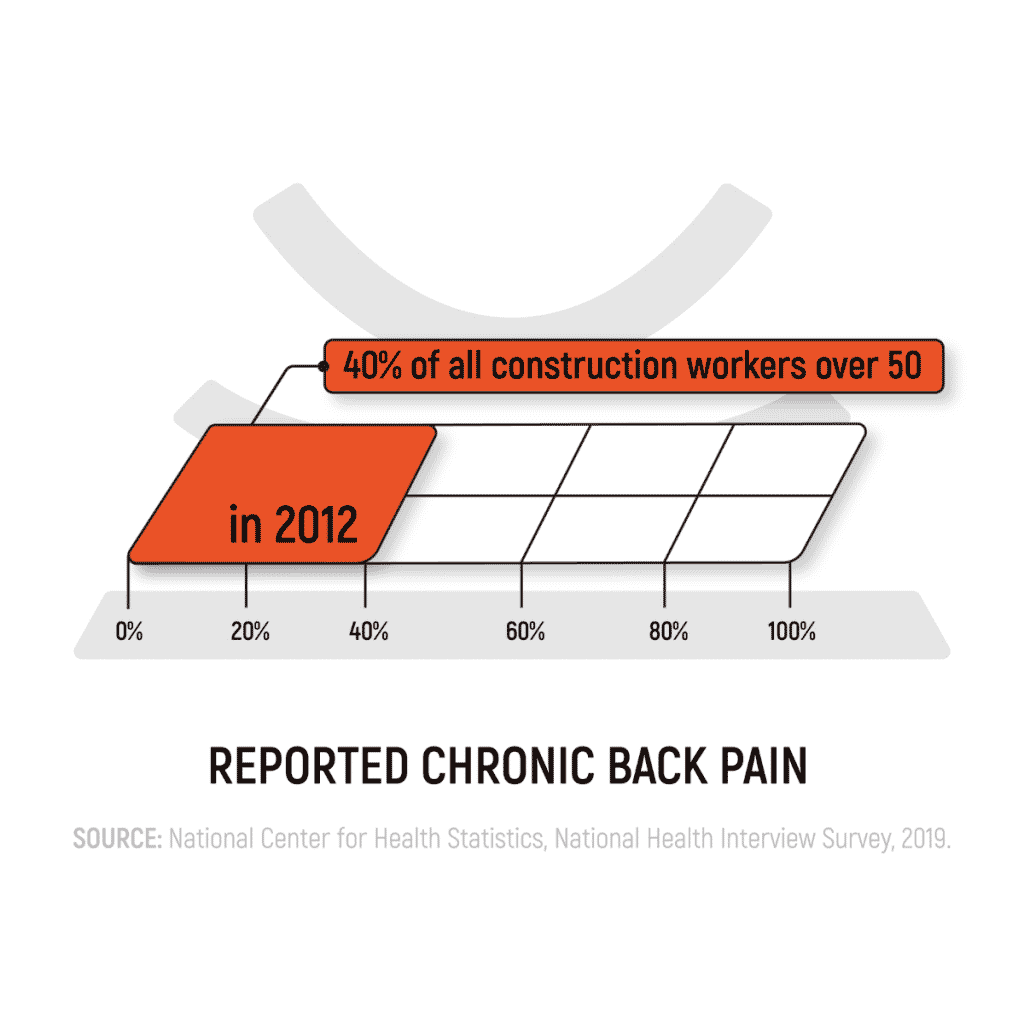
It’s also possible that physically demanding jobs can lead to chronic pain. For example, a study done in 2012 reported that 40% of all construction workers over 50 reported chronic pain, the majority of which was back pain.
Common Treatments for Chronic Pain
There are several treatments for chronic pain, ranging from non-steroidal anti-inflammatory drugs (NSAIDS) to prescription painkillers and physical therapy. We’ll discuss the other options below and briefly note their efficacy.
Over-the-Counter Medicine
Over-the-counter (OTC) medicine is used, at least for some time, to treat most instances of chronic pain. Chronic pain begins as acute pain — lasting less than four weeks — so most individuals resort to over-the-counter medicine for a while.
These medications are easy to acquire and present little to no risk with short-term use. However, they are significantly more risky with prolonged use, so while they may provide temporary relief for chronic pain, they shouldn’t be considered a long-term solution.
Some of the most common OTC medications for acute and chronic pain are listed below:
- Acetaminophen (Tylenol)
- Aspirin
- Ibuprofen (Advil, Motrin)
- Naproxen (Aleve)
Prescription Medicine
As is typically the case, prescription medicine is far more effective than OTC options for treating chronic pain. However, many prescription medications are also inherently more dangerous, as some come with more severe side effects and a higher risk of dependency.
Specifically, opioids treat severe pain, but they can be highly addictive.
Some of the most common prescription medications used to treat chronic pain are listed below:
- COX-2 inhibitors, like Celecoxib (Celebrex, Consensi) [these are particularly effective because they provide the same anti-inflammatory and pain-reducing effects as NSAIDs but without many of the common and more dangerous side effects]
- Antidepressants like amitriptyline and nortriptyline (Pamelor), venlafaxine (Pristiq, Effexor), duloxetine (Cymbalta), and milnacipran (Savella, Fetzima)
- Anti-seizure medications are sometimes used in more extreme cases, such as fibromyalgia or chronic nerve pain. These include pregabalin (Lyrica) and gabapentin (Neurontin, Horizant, Gralise)
- Opioids, although these come with some of the highest risks of dependency. These include hydrocodone (Vicodin, Norco, Lortab), hydrocodone-acetaminophen (Vicodin, Lortab, Lorcet, Norco, Xodol), oxycodone (Oxycontin, OxyIR, OxyFast), and oxycodone-acetaminophen (Percocet, Primlev, Endocet, Roxicet, Tylox, Xartemis)
Physical Therapy & Chiropractic Medicine
In some cases, usually depending on the reason the individual is experiencing chronic pain, physical therapy, and chiropractic medicine can be used as treatments. Often, these options are used in combination with OTC or prescription medications as a part of a pain management program.
Physical therapy aims to treat acute and chronic pain and provide better mobility, strength, and blood flow in the affected area. This can be an outstanding way to treat chronic pain, especially when combined with other pain management techniques.
Physical therapy often provides patients with a means of dealing with their chronic pain outside of treatment with home exercise and stretching programs to help provide pain relief outside of the clinical setting. It can be a great way to treat muscle and joint pain and can even be highly effective for treating nerve pain in some instances.
Chiropractors offer more immediate relief for some individuals with chronic pain, but only in some instances. Chiropractic treatment involves physical manipulations of joints throughout the body to provide better mobility. In some cases, it can help treat chronic pain that results from traumatic injuries. There is not much research to suggest that chiropractic medicine is a viable solution for chronic pain, although some individuals find relief with treatment.

Alternative Medicine
There are quite a few alternative methods for treating chronic pain, from acupuncture and guided meditation to natural remedies like capsaicin and essential oils. Growing evidence suggests that alternative medicine is legitimately effective, and these methods have been used in traditional medicine for hundreds of years.
However, many people believe that any positive effect of alternative medicine is purely psychological — although a placebo effect that effectively gets rid of chronic pain should be considered as effective as any other method.
Kratom for Chronic Pain
Many people over the past decade or so have been turning to kratom, which comes from the Mitragyna speciosa tree. This tree grows naturally in Southeast Asia, specifically in Indonesia. The leaves are dried and crushed, then consumed as a dry powder or mixed with water or other beverage.
Kratom contains alkaloids — namely mitragynine and 7-hydroxymitragynine — that interact with the opioid receptors. Specifically, mitragynine binds to μ-opioid receptors, which block pain signals traveling in the central nervous system before they reach the brain [4]. In addition to negative feelings like pain, these same receptors handle positive feelings like euphoria. As such, mitragynine can provide mental relief to those suffering from depression and anxiety caused by chronic pain.
Similarly, 7-hydroxymitragynine binds to alpha-opioid receptors and other opioid receptors [5]. These receptors also play a role in our perception of pain, which means 7-hydroxymitragynine can also help block pain signals that reach the brain. While these receptors are bound to the alkaloids in kratom, they are unable to respond to pain signals, which provides a feeling of relief, even from more severe nerve pain in some cases.
Contrary to popular belief, kratom is not an opioid, although it does similarly interact with the body. Kratom is safer than opioids because it is far less addictive than many prescription medications. There is still a risk of dependency, although most users can keep the risk of addiction to a minimum by taking breaks and minimizing their daily dosages.
Related: Is Pain Really Necessary? Yes — Here’s Why & What You Can Do About It

Chronic Pain Statistics
With the prevalence of chronic pain in America and throughout the world, plenty of statistics are available about who lives with chronic pain, why they experience it, and how it is treated.
We’ll provide some of the most interesting chronic pain statistics below.
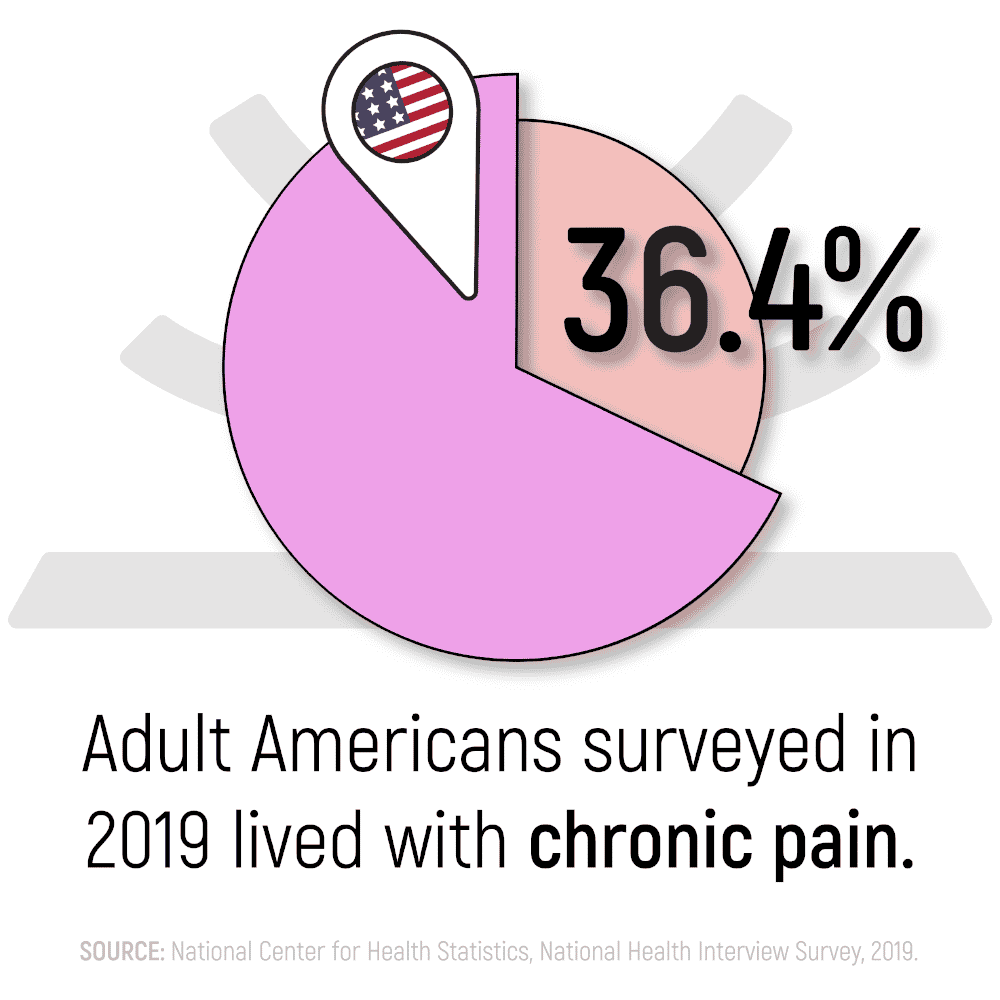
- A study done in 2019 confirmed that 20.4% of adults had chronic pain at the time of the survey.
- That same study showed that more than 7% of respondents had “high impact chronic pain,” which is defined as chronic pain that severely limits normal function, including walking, working, and social gathering.
- Chronic pain and high-impact chronic pain are both more prevalent in older populations.
- Chronic pain is more common in rural and suburban areas than in urban areas, possibly due to the differences in overall mindset or the quality of healthcare.
- Chronic pain is most common in non-Hispanic white individuals than in those who identify as black, Hispanic, and Asian.
- Chronic pain is one of the most common reasons individuals seek medical attention [6].
- Chronic pain often leads to issues with mental health, including depression, anxiety, and drug addiction [7, 8].
- About 20% of all American individuals will, at some point, experience chronic pain.
- Most individuals living with high-impact chronic pain find it impossible to work outside their homes.
- Chronic pain is the leading cause of disability in the United States [9].
- Around 54% of all Americans have dealt with chronic pain for five years or longer.

- Lower tiers of education seem to be related to higher instances of chronic pain, with the highest instance in individuals with no more than high school education.
- Certain socioeconomic factors — like low income or social status — tend to correlate with a higher risk of chronic pain.
- Between 3 and 5% of all Americans cope with chronic migraines.
- Chronic neuropathic pain — such as fibromyalgia and diabetic neuropathy — is something as much as 17% of the population deals with daily [10]
- Around 7% of the US population reports chronic pain due to arthritis.
- Arthritis is significantly more likely to occur in women than in men.
- Surprisingly, arthritis is reported least often by adults over 65 and most often by those between 45 and 64.
- Obesity is associated with significantly higher rates of arthritis and resulting chronic pain.
- The large majority of cancer patients — about 70% — cope with chronic pain.
- Just under half of all cancer patients reportedly cope with neuropathic pain.
- A Harvard study suggests that individuals with chronic pain are more likely to become depressed, experience anxiety and stress, and live with other mental health issues.
- Opioid misuse occurs in more than a quarter of all patients who take prescription drugs to manage chronic pain.
- More than 17,000 deaths annually are attributed to opioid overdose, many of which stem from opioid use to treat chronic pain.

- 73% of individuals who have dealt with chronic pain have used non-steroidal anti-inflammatory drugs (NSAIDs) for treatment.
- Chronic pain is responsible for more than half a trillion dollars annually in healthcare costs and estimated losses experienced by companies with employees who take off because of chronic pain.
- Chronic pain is one of the most costly ailments in America regarding healthcare costs.
- Individuals coping with chronic pain pay far more in medical bills every year — nearly $5,000 more — than individuals who aren’t experiencing chronic pain.
- Prescription medications are only effective for treating slightly more than half of the instances of chronic pain they’re used to treat.
- Chronic pain affects sleep negatively, and a lack of sleep is sometimes linked to an increased risk of chronic pain. This causes a positive feedback cycle that can perpetuate chronic pain.
- Chronic pain conditions in 2018 were diagnosed most in individuals over 65. Younger patients are less likely to experience chronic pain overall.
- A 2017 study revealed that more than half of the respondents had dealt with chronic pain related to neck or back issues.
- Only about 10% of all individuals who deal with chronic pain will experience it for three years or less.

- Arthritis and related chronic pain are some of the most commonly reported health issues among veterans.
- The prevalence of chronic pain is about equal among individuals with education levels lower than high school, those with a high school degree or GED, and those with some college education. The prevalence dips in individuals with a bachelor’s degree and continues to decrease with higher education.
- Chronic pain is most common in individuals aged 45 to 64, as is high-impact chronic pain.
- Chronic pain is about 33% more common in women than in men. High-impact chronic pain is about 25% more common in women than in men.
- Chronic pain related to joint pain is the most common chronic pain condition to be treated with opioids, followed by back pain, neck pain, and head pain.

- Nearly half of all individuals who use opioids long-term take them for joint pain.
The Most Prevalent Type of Chronic Pain
Among individuals who cope with chronic pain on a daily basis, back pain is the most prevalent. The 2019 study conducted by the CDC mentioned above also found that an incredible 39% of all study participants reported having dealt with chronic back pain in the three months leading up to the survey. Chronic lower limb pain and chronic upper limb pain were reportedly less common, at 36.5% and 30.7%, respectively.
The prevalence of back pain was highest in all groups prone to chronic pain in general. These groups included elderly individuals, those living below the federal poverty line, women, and non-Hispanic whites.
Back Pain Statistics
Below, we’ll share some interesting statistics about back pain, including who it affects, how prevalent it is, and the consequences of such a high rate of occurrence.
- A study from Georgetown University found that back pain was the leading cause of missed work days in the year leading up to the survey.
- An incredible 13.7% of acute back pain instances are treated with opioids, despite a lack of evidence that it is an effective treatment.
- Americans miss approximately 83 million days of work annually because of chronic back pain [11].
- About 18% of Americans sought medical attention for lower back pain in 2018.
- Lower back pain was nearly twice as prevalent in 2017 than it was in 1990 [12].
- About three-quarters of Americans with chronic back pain are in otherwise good physical health.
- Chronic back pain leads to psychological issues, including depression and anxiety.
- Chronic lower back pain is more common in females than in males [2].
- Back pain is one of the top three most common reasons Americans visit their doctors, behind skin issues and joint problems [13].
- The health care expenses for adults with chronic back pain are more than double that of adults without chronic back pain.
- Lower back pain is more often caused by isolated events than medical conditions, including arthritis [14].
- Adults with chronic back pain report being severely socially and physically limited.
- Elderly adults with back pain report lower feelings of happiness in retirement than those without it.
- The number of years individuals live with chronic back pain has increased significantly — over 50% — from 1990 to 2015 [14].
- More adults without back pain are a part of the labor force than those with chronic back pain.
- Approximately $50 million yearly in healthcare costs are associated with chronic back pain.
- Chronic back pain is the most common cause of disability in the United States [15].
- Adults who continue to work while living with back pain statistically earn about two-thirds of those who work without chronic back pain.
- More than a quarter of all chronic back pain patients believe that stress is the cause of their ailment.
- About 20% of chronic back pain patients believe that sitting all day at work has affected their pain levels.

Wrapping Up
Chronic pain — defined as pain lasting for longer than three months — is a severe condition in America and worldwide. Individuals can experience chronic pain in any portion of the body, although back and neck pain is most common, followed by limb pain. Chronic pain can be triggered by traumatic injuries, psychosomatic illnesses, repeated strain injuries, and more.
Chronic pain tends to be more prevalent in older populations, women, and non-Hispanic white individuals. It also is correlated with lower education, social status, and income, especially when income levels are below the federal poverty line.
Although chronic pain can often seem like a hopeless situation, many different solutions and treatments can help manage the pain or eliminate it entirely. Some of the most common answers are over-the-counter medications, prescription medications, physical therapy, chiropractic medicine, alternative medicine, and natural remedies like kratom.
- 3De Souza, I. M. B., Sakaguchi, T. F., Yuan, S. L. K., Matsutani, L. A., do Espírito-Santo, A. D. S., Pereira, C. A. D. B., & Marques, A. P. (2019). Prevalence of low back pain in the elderly population: a systematic review. Clinics, 74.
- Anderson, A. S., & Loeser, R. F. (2010). Why is osteoarthritis an age-related disease?. Best practice & research Clinical rheumatology, 24(1), 15-26.
- Sluka, K. A., O’Donnell, J. M., Danielson, J., & Rasmussen, L. A. (2013). Regular physical activity prevents development of chronic pain and activation of central neurons. Journal of applied physiology, 114(6), 725-733.
- Suhaimi, F. W., Yusoff, N. H., Hassan, R., Mansor, S. M., Navaratnam, V., Müller, C. P., & Hassan, Z. (2016). Neurobiology of Kratom and its main alkaloid mitragynine. Brain research bulletin, 126, 29-40.
- Matsumoto, K., Horie, S., Ishikawa, H., Takayama, H., Aimi, N., Ponglux, D., & Watanabe, K. (2004). Antinociceptive effect of 7-hydroxymitragynine in mice: Discovery of an orally active opioid analgesic from the Thai medicinal herb Mitragyna speciosa. Life sciences, 74(17), 2143-2155.
- Schappert, S. M. (1999). Ambulatory care visits to physician offices, hospital outpatient departments, and emergency departments: United States, 1997.
- Pizzo, P. A., Clark, N. M., & Carter-Pokras, O. (2011). Relieving pain in America: A blueprint for transforming prevention, care, education, and research. Institute of Medicine, 382.
- Smith, B. H., Elliott, A. M., Chambers, W. A., Smith, W. C., Hannaford, P. C., & Penny, K. (2001). The impact of chronic pain in the community. Family practice, 18(3), 292-299.
- Mills, S. E., Nicolson, K. P., & Smith, B. H. (2019). Chronic pain: a review of its epidemiology and associated factors in population-based studies. British journal of anaesthesia, 123(2), e273-e283.
- Cavalli, E., Mammana, S., Nicoletti, F., Bramanti, P., & Mazzon, E. (2019). The neuropathic pain: An overview of the current treatment and future therapeutic approaches. International Journal of Immunopathology and Pharmacology, 33, 2058738419838383.
- Druss, B. G., Marcus, S. C., Olfson, M., & Pincus, H. A. (2002). The most expensive medical conditions in America. Health affairs, 21(4), 105-111.
- Wu, A., March, L., Zheng, X., Huang, J., Wang, X., Zhao, J., … & Hoy, D. (2020). Global low back pain prevalence and years lived with disability from 1990 to 2017: estimates from the Global Burden of Disease Study 2017. Annals of translational medicine, 8(6).
- Sauver, J. L. S., Warner, D. O., Yawn, B. P., Jacobson, D. J., McGree, M. E., Pankratz, J. J., … & Rocca, W. A. (2013, January). Why patients visit their doctors: assessing the most prevalent conditions in a defined American population. In Mayo Clinic Proceedings (Vol. 88, No. 1, pp. 56-67). Elsevier.
- Hartvigsen, J., Hancock, M. J., Kongsted, A., Louw, Q., Ferreira, M. L., Genevay, S., … & Woolf, A. (2018). What low back pain is and why we need to pay attention. The Lancet, 391(10137), 2356-2367.
- Hoy, D., March, L., Brooks, P., Blyth, F., Woolf, A., Bain, C., … & Buchbinder, R. (2014). The global burden of low back pain: estimates from the Global Burden of Disease 2010 study. Annals of the rheumatic diseases, 73(6), 968-974.