Kratom, Opioids, & Itching: How Are They Linked?
Itching is one of the most irritating side effects caused by opioids of any type.
The relentless itching can make it impossible to sit still. Sometimes the itching is so intense people can’t sleep. Some recreational users even enjoy itching since this often indicates a very high dose.
Itching tends to occur when you’re really, really high. The stronger the buzz, the stronger the itch.
Kratom is not quite an opioid — it’s technically an atypical opioid and has a similar mechanism of action.

It’s been many years since I’ve gotten an itch from kratom. I attribute that mostly to tolerance, although even after a six-month break, I was completely unable to get another itch. It was my first few times using a strong red when I got itchy.
But it turns out that the pharmacology of opioid-related itching is quite complex, much more so than most of the community is aware of.
Opioid Receptors & Itching
Opioids affect the body’s histamine production in different ways [1]. However, most opioids interact with the immune system similarly to certain allergens, triggering the mast cell cascade and the release of histamine.
One would assume that this is the cause of opioid-related itching. However, the study above shows that animals deficient in mast cells still respond to opioid receptor-related itch.
And, while morphine use does cause an acute rise in histamine levels, they return to baseline within an hour [2]. Many people don’t begin to experience itching until several hours after a dose.

It’s important to note that there are three subsets of opioid receptors: mu, delta, and kappa. The mu-opioid receptor is the most powerful one.
By some mechanism, mu-opioid agonism (activation) seems to elicit the itching response directly.
Kratom, the Atypical Opioid
Mitragynine and the more potent 7-hydroxymitragynine are kratom’s main active opioid-like alkaloids. Research shows the latter is much more potent than morphine, though kratom has minuscule amounts of each [3].
Strains high in this alkaloid — usually red-veined strains — tend to produce more itching than other types of kratom. Also, as people become tolerant to kratom, they tend to experience less itching.
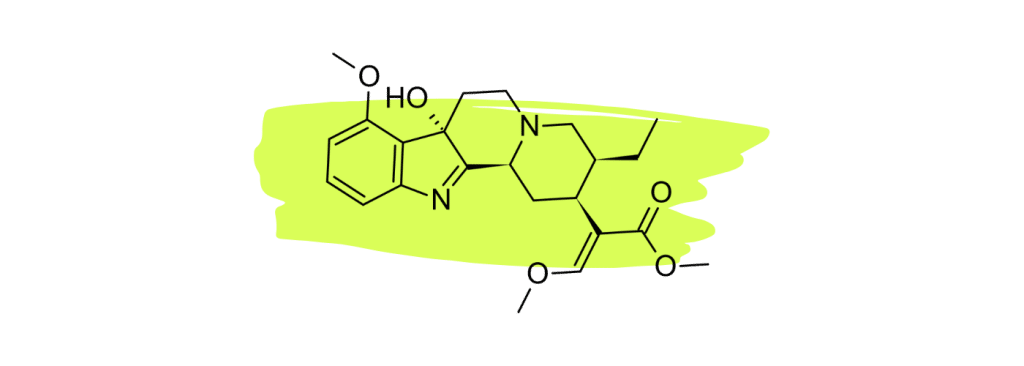
Nonetheless, these alkaloids follow a similar mechanism of action as any other opioid. However, there may be some changes in the specifics regarding which cells they interact with and how strongly.
Histamine & Itching
There’s a lot of confusion in the world of opioid users and kratom enthusiasts regarding the role of histamine and itching.
Itching is a side effect that comes directly from the histamine system. Histamine is a compound the body produces in an allergic reaction. Symptoms of histamine release include itching, of course, as well as watery eyes, runny nose, sneezing, and hives.
Most people would like to think that it’s as simple as “histamine release causes itching,” but if that were the case, then popping an antihistamine would eliminate itching.
While antihistamines are generally effective, they don’t work for everyone, and part of the reason for that is the complexity of the histamine system.

When it comes to allergic reactions, a complex chain reaction of immune cells causes histamine release.
- The body’s antigen-presenting cells (APCs) detect the allergen.
- APCs activate immune T cells.
- The T cells release B cells which identify the antibodies present on the invading compound and begin to produce antibodies of their own, capable of attaching to the antigen’s antibodies.
- Antibodies stick to the antigen, which then sticks to mast cells.
- Once the antigen is stuck to the mast cell and the antibodies are activated, the mast cell degranulates and releases many different compounds, including cytokines (inflammatory markers) and histamine.
- These compounds produce the symptoms of allergies that we’re familiar with: itching, inflammation, hives, and so on.
If life were easy, this knowledge would be enough for us to overcome opioid-induced itching. But it’s not.
Choline & Itching
The experiences of individuals and the current research agree that mu-opioid agonists lead to allergy-like reactions like itching in opiate users.
What is really interesting is how these histamine-like symptoms tend to continue once someone stops using kratom or other opioids.
Stopping the use of an addictive substance can cause the body to go through withdrawal symptoms — kratom is no different.
Using kratom tends to make people feel euphoric and productive, chatty, anxiety-free, comfortable in their bodies, and full of energy (with greens or whites) or find long-deserved relief from pain (with reds). It can also cause itching, a symptom reminiscent of an allergy.
Withdrawal symptoms are respectively the opposite of such symptoms: people feel depressed and unmotivated, antisocial, anxiety-ridden, uncomfortable, and incapable of accomplishing anything or even desiring to.
Physically, some of the major symptoms of withdrawal are allergy-like — suggesting histamine release.
Histamine release isn’t responsible for the allergy-like withdrawal symptoms of opioid withdrawal.
Interestingly, opioids themselves also function as anticholinergics. In other words, they suppress the body’s production of choline. Antihistamines also work as anticholinergics.
Anticholinergic effects are a general slowing down of the nervous system and can cause the following:
- Sluggishness, both physical and mental
- Difficulty urinating and slowed digestive motility, leading to constipation
- Dry mouth and dry skin, often attributed to dehydration
- Confusion and slow thinking
Choline also helps regulate our breathing rate and the sensation of pain.
As discussed earlier, withdrawal symptoms tend to take the form of the equal and opposite effects of the addictive symptoms. Anticholinergic drugs lead to a cholinergic rebound, which causes extremely uncomfortable symptoms.
On the mild end, these symptoms can be reminiscent of a cold: runny nose and eyes, yawning, and feeling fatigued yet restless.
More serious symptoms result from the nervous system functioning in overdrive and include chills, shaking, restless leg syndrome, and increased pain sensitivity.
This is important to note because it can influence your decision regarding some of the common treatments used for kratom itch.
Skin Cells & Itching
The mu-opioid receptor expresses itself on a number of different skin cells. These include keratinocytes, fibroblasts, immune cells, and sensory neurons, all of which are capable of producing an itching response directly.
The human body’s various mast cells also seem to react differently to morphine [4]. For example, those found in the skin will degranulate and release histamine when exposed to morphine. However, the same cells found in the lungs, heart, or intestines will not.
As it turns out, mast cells are hardly the only cells or channels in the human body programmed to produce an itching response. Researchers have discovered nearly a dozen of these so far [5].
The transient receptor potential vanilloid 1 (TRPV-1) channel is particularly interesting to kratom users. Remember, opioid receptors themselves are prurogenic (itch-producing) receptors.
Some researchers believe that the relationship between the mu-opioid receptors found on the TRPV-1 channel causes this itch. These opioid receptors are particularly dense in their expression among TRPV-1.
However, despite TRPV-1 being highly involved in the itch response, especially when involving histamines, the study revealed that mice completely devoid of TRPV-1 still experienced itching when receiving a dose of the DAMGA agonist [6]. Instead, the study showed that nerve fibers that produce TRPV-1 are responsible for the itching mechanism.
This conclusion — drawn through a series of horrific experiments involving the dissemination of various nerve cells through repeated injections of multiple chemicals — probably did little for the advancement of humanity. The result is limited to the discovery of non-peptogenic TRPV-1-expressing C fibers causing an opiate itch in rats.
How Can I Prevent Kratom Itch?
It disappoints many people to find out that topical anti-itch creams do nothing for their kratom itch. That’s because the itch isn’t a surface-level issue.
1. Antihistamines
It’s caused by the stimulation of neural fibers within your body, and the only way to stop it is to inhibit that particular biological action. The easiest way to do this is to use antihistamines.
The most common of these are:
- Diphenhydramine (Benadryl)
- Dimenhydrinate (Dramamine or Gravol; this is a prodrug that becomes diphenhydramine)
- Doxylamine (Vick’s NyQuil)
- Azelastine (Astelin)
- Loratadine (Claritin)
- Cetirizine (Zyrtec)
- Desloratadine (Clarinex)
- Fexofenadine (Allegra)
All these drugs are usually very effective at reducing kratom itch — some are also powerful sedatives and need to be used carefully.
We don’t recommend combining antihistamines with kratom or opioids — especially first-generation antihistamines like diphenhydramine, diphenhydrinate, and doxylamine.
It’s important to remember, too, that antihistamine drugs like these are usually potent anticholinergics. They will significantly increase the anticholinergic effects that kratom already causes, even though they might reduce your itching.
That means that you run the risk of compounding withdrawal symptoms when you stop using kratom. At most, you should use anticholinergics every few days. The best-case scenario would be not to use these at all if possible, but if the itching is too much, they can be a great help.
Though taking an anticholinergic drug during a cholinergic rebound might make sense, these drugs also tend to suppress dopamine.
This can aggravate symptoms like restless legs, and many people have reported nightmare experiences after popping a Benadryl or two in hopes of sleeping.
2. Opioid Receptors
Kappa opioid agonism is unique in that it tends to produce effects that are the opposite of mu stimulation (including dysphoria, discomfort, hallucinations, and restlessness) and can also reverse itching [7].
This is particularly interesting because highly selective, potent mu-opioid agonist drugs — substances that target this particular receptor and do very little else — cause an itching effect that is reversible with naloxone.
Naloxone is an opioid antagonist that occupies opioid receptor sites but does not activate them. It is nothing like an antihistamine. If itching were caused by histamine release alone, then an antihistamine would be the sort of drug you would expect to stop it — not a drug that prevents opiate activity.

Nonetheless, mice injected with the selective mu agonist DAMGA had their itching symptoms entirely reversed by naloxone [8]. This was the first suggestion that something else was taking place other than a simple histamine release.
Another study in Science Daily, this one from 2011, revealed some promising information. The researchers experimented using their knowledge of the various subtypes of opioid receptors.
One subtype, called the mu-opioid receptor 1D (MOR1D), seems to be directly responsible for itching. This appears to operate separately from the mechanism of the previous study.
When the researchers deactivated this opioid receptor subtype in the spinal cord of mice, they immediately stopped itching. Gastrin-releasing peptide receptors (GRPRs) transmit itching information through the nervous system but do not transmit pain information.
MOR1D receptors activate GRPRs, sending itching signals, but deactivation is possible. Additionally, it doesn’t interfere with the painkilling benefits of morphine at all.
3. Choline
Research shows that citicoline, the dietetic source of choline, could be a treatment for addiction by decreasing cravings and withdrawal symptoms and improving cognitive functioning [9].
A choline supplement can bring the levels into a normal range and help offset the impact of the antihistamines’ and opioids’ anticholinergic effects.
Is Kratom Itching Dangerous?
The itching itself isn’t dangerous. It’s a normal and quite typical response to the body’s exposure to opioid chemicals. However, itching generally indicates (at least with kratom) that you’ve taken a relatively high dose.
While there’s little risk of overdosing on kratom, itching usually indicates that you’re approaching the threshold.

Due to the lack of regulation in the kratom industry, there’s nothing stopping vendors from adulterating their kratom with a synthetic opioid so they can have a stronger product. Such was the case with Krypton Kratom, a product that might have contained the synthetic opioid O-desmethyltramadol.
In this case, the danger is not from kratom but other substances the user is unaware of. Combining kratom with other substances can cause dangerous interactions and is one of the most significant risks.
Be especially careful if you’re using potentiators to enhance kratom. These can easily throw you into different territory, decimating the line between “just right” and “way too much.”
Again, kratom overdoses are rare and usually aren’t fatal, but they’re not safe and will certainly not help kratom’s already fragile image.
Final Thoughts on Kratom Itches
Kratom itches are certainly a relic of my past, as are the all-encompassing blissful states of complete couch-lock that came with them. While a big part of me misses the experience of being itchy, I’m glad it’s not the focal point of my existence anymore.
Regardless of what people say, kratom — and opioids in general — can mess up your equilibrium. Whether that means jacking up the production of enzyme x or preventing the synthesis of hormone y, it ultimately takes a toll.
Just because the symptoms aren’t as obvious or debilitating as something like a crippling heroin addiction doesn’t mean that it’s wise to treat your body like this.
So, for now, I’m going to revel in the fact that I’m not insatiably itchy. Instead of reassuring myself with every new pin-prick itch that I’m high as a dog at the vet, I’ll reassure myself every second I’m not scratching that my hormones are working in balance once again.
- Melo, H., Basso, L., Iftinca, M., MacNaughton, W. K., Hollenberg, M. D., McKay, D. M., & Altier, C. (2018). Itch induced by peripheral mu opioid receptors is dependent on TRPV1-expressing neurons and alleviated by channel activation. Scientific reports, 8(1), 1-9.
- McBride, P., Jacobs, R., Bradley, D., & Kaliner, M. (1989). Use of plasma histamine levels to monitor cutaneous mast cell degranulation. Journal of allergy and clinical immunology, 83(2), 374-380.
- Matsumoto, K., Hatori, Y., Murayama, T., Tashima, K., Wongseripipatana, S., Misawa, K., … & Horie, S. (2006). Involvement of μ-opioid receptors in antinociception and inhibition of gastrointestinal transit induced by 7-hydroxymitragynine, isolated from Thai herbal medicine Mitragyna speciosa. European journal of pharmacology, 549(1-3), 63-70.
- Stellato, C., Cirillo, R., de Paulis, A., Casolaro, V., Patella, V., Mastronardi, P., … & Marone, G. (1992, November). Human basophil/mast cell releasability: IX. Heterogeneity of the effects of opioids on mediator release. In The Journal of the American Society of Anesthesiologists (Vol. 77, No. 5, pp. 932-940). The American Society of Anesthesiologists.
- Bautista, D. M., Wilson, S. R., & Hoon, M. A. (2014). Why we scratch an itch: the molecules, cells and circuits of itch. Nature neuroscience, 17(2), 175-182.
- Imamachi, N., Park, G. H., Lee, H., Anderson, D. J., Simon, M. I., Basbaum, A. I., & Han, S. K. (2009). TRPV1-expressing primary afferents generate behavioral responses to pruritogens via multiple mechanisms. Proceedings of the National Academy of Sciences, 106(27), 11330-11335.
- Phan, N. Q., Lotts, T., Antal, A., Bernhard, J. D., & Ständer, S. (2012). Systemic kappa opioid receptor agonists in the treatment of chronic pruritus: a literature review. Acta dermato-venereologica, 92(5), 555-560.
- Yamamoto, A., & Sugimoto, Y. (2010). Involvement of peripheral mu opioid receptors in scratching behavior in mice. European journal of pharmacology, 649(1-3), 336-341.
- Wignall, N. D., & Brown, E. S. (2014). Citicoline in addictive disorders: a review of the literature. The American journal of drug and alcohol abuse, 40(4), 262-268.